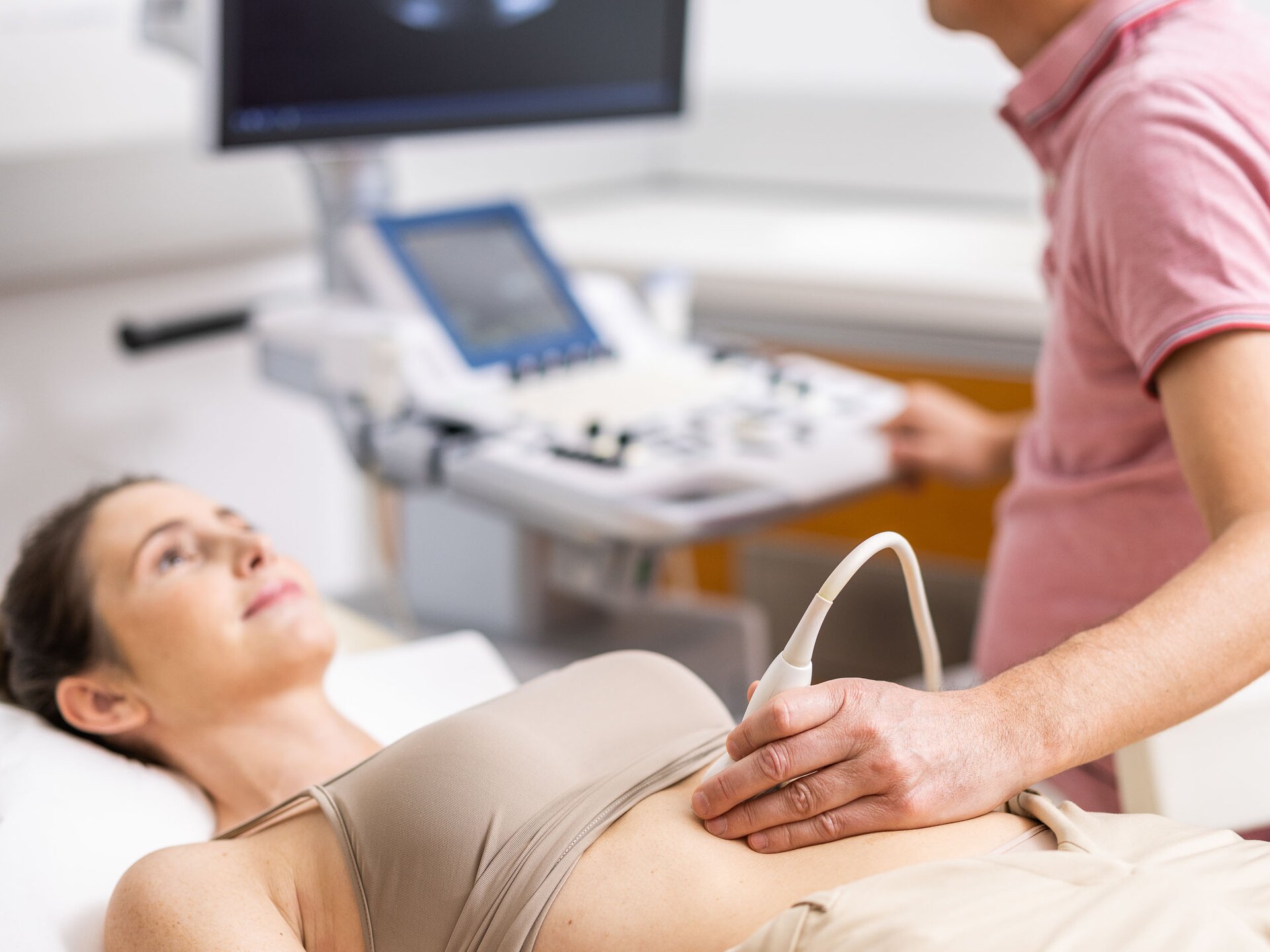
Medical Spa Resort near Innsbruck
Park Igls
Relaxed. Rejuvenated. Revitalised. Stays at the Park Igls Medical Spa Resort, perched on a high plateau above the city of Innsbruck, have a lasting, sustainable effect on guests' health. The fundamentals of Modern Mayr Medicine are combined with extensive expertise from a range of specialist doctors, discreet personal service and comprehensive infrastructure to create a made-to-measure experience tailored to each and every guest's specific needs.
21 to 28 April 2024 (in German) 25 August to 01 September 2024 (in German) 18 August to 25 August 2024 (in English)
from € 3.671 per person
Well prepared and informed
The Park-Igls-App
Learn all about your stay, find interesting resort-facts, daily and weekly programmes, regional tips and much more. Take a look at the world of the Park Igls Medical Spa Resort while you are still at home.
Your vote for the 2025 Awards
Condé Nast Johansens
As a long-standing winner of the Condé Nast Johansen Awards, we know that our satisfied guests are the most important part of a successful overall rating. If you value the Park Igls, then we look forward to your vote in one of the recommended categories and would like to say thank you!
- Best Value Experience
- Best Destination Spa
- Best Treatment Menu






Programmes and specials at the Park Igls Medical Spa Resort
As individual as you
Here at Park Igls we have spent years perfecting our programmes in order to offer individual solutions to the mental and physical challenges posed by today's society. Modern Mayr Medicine offers the ideal basis for sustainable prevention and regeneration, combining holistic therapies and diagnostics with specific nutrition and exercise.
The truth about the Mayr Cure
Debunking some common Mayr myths
No. Don't worry! Here at Park Igls we only use this approach for dietary stage 1, but many guests begin their stay at dietary stage 2 (including a protein supplement). The conscious initial reduction of foods for cleansing and detoxification creates the foundation. Building on this, we then establish a balanced and healthy diet. With your sense of taste refreshed and rejuvenated, the excellent Mayr Cuisine at Park Igls invites you to discover a whole world of fascinating tastes and sensations.
To ensure that your time-out with us does not remain a one-off experience, our medical staff will support you right from the start in developing a concept that is suitable for the stress, strain and time pressure of everyday life. We are convinced that a single stay or one-off solution is not enough for healthy, sustainable lifestyle. True healthy living only comes about we make the right decisions day by day, no matter how small they may be.
It is, as the saying goes, a question of taste. The dietary plans we follow at Park Igls have been carefully developed to combine regional, organic and fresh produce in creative meals drawing on the expertise of our outstanding team of chefs. We are sure you and your tastebuds won't find the food on offer here boring or bland.
Yes. This is backed up, on the one hand, by our team of qualified specialists and, on the other hand, by scientific studies and treatment successes over more than a century. Modern Mayr Medicine is recognised worldwide and has been practised and optimised at the Park Igls Medical Spa Resort for many years.
Yes. At the beginning of a stay at Park Igls, your personal supervising doctor will sit down with you and ask in detail about your personal wishes, needs and situation. Together you will create the ideal programme for your body and mind. A network of doctors from many specialties from Innsbruck and the surrounding area work together in our health centre for your well-being.
Sorry to disappoint you, but the answer is no. "Fast" is a word which doesn't exist in the F. X. Mayr Cure. Changing your life is always a process – one which has been practised and optimised here at Park Igls for decades. You will find some general recommendations and advice in our blog, but change that is effective in the long term is most successful when it is supported and guided by experienced experts.
Modern Mayr Cuisine
Fasting
Think Park Igls is simply a fasting hotel in Austria? Time to think again! We invite you to take a look behind the scenes and discover how healthy eating and fasting do not have to be synonymous with bland, boring meals. On the contrary, Modern Mayr Cuisine is a conscious way of controlling food intake while at the same time enjoying the pleasure of eating.
Interviews with experts, delicious recipes, tips, ideas and much more!
Enjoy the Park Igls experience at home
Recipes, recommendations, ideas
Health blog
Highest quality for highest demands
In Short
The four pillars of Modern Mayr Medicine
A holistic view of health
Prizes, awards, excellent ratings and top reviews in international media
The Park Igls seal of approval
Read our magazine online
Winter ParkZeit
Our publication "ParkZeit" presents current topics from our Resort in a compact and entertaining way. In addition to informative stories, you will also learn interesting facts about our spa and therapy programme. You can read the current issue online.
Please don't hesitate to get in touch if you have any questions or queries. We look forward to hearing from you.